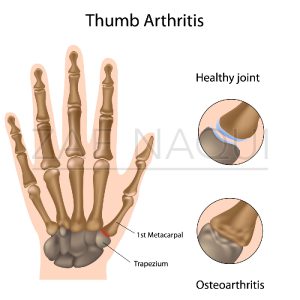
Base of Thumb Osteoarthritis

What is it?
Normally the bone surfaces in the wrist are lined with cartilage, which allows smooth movements between the base of the thumb and the wrist bone (trapezium). In base of thumb osteoarthritis (OA) the cartilage degenerates or wears out and the movement between the joints becomes painful as the bony surfaces are now in contact with each other.
Who gets it and what causes it?
This condition usually affects middle aged to elderly persons. There is no known direct cause but there are links with previous fractures or dislocations of the wrist and joint laxity. The base of the thumb and the hip are the two most frequent sites of Osteoarthritis in the body.
What are the signs and symptoms?
The main symptom is pain at the thumb base, which may be very severe especially when undertaking tasks that involve pinching type movements e.g. holding a pen. Intricate movements of the hand and thumb. Weakness, deformity and swelling may also develop around the joint in advanced cases.
What tests will I need?
Following a consultation, involving a medical history and clinical examination, an X-ray will be taken of your hand(s).
What is the treatment?
Initially Mr. Naqui will attempt conservative measures such as regular painkillers and occasional steroid injections into the joint. Splinting of the wrist and hand therapist directed exercises can also help. Persistent or severe symptoms are likely to require surgical treatment.
What does the surgical treatment involve?
There are a number of different treatment options including joint fusion, removal and ligament reconstruction (arthroplasty).
In joint fusion the joint surfaces between the base of thumb and wrist bone (trapezium) are fused. This prevents any movement at the joint and hence prevents the bones from rubbing against each other and causing pain. This procedure is more commonly performed in younger patients with manual worker type jobs.
In joint removal and ligament reconstruction, the trapezium bone (which is normally in contact with the base of the thumb) is removed and replaced with a strip of tendon.
Mr. Naqui performs base of thumb OA surgery at a number of hospitals around Manchester, see Hospitals page. The surgery usually lasts 45 minutes and is a day case procedure requiring regional or general anaesthetic, see FAQs page. The surgical scar is usually 4 to 5cm long. A plaster of Paris splint will be applied at the end of your surgery.
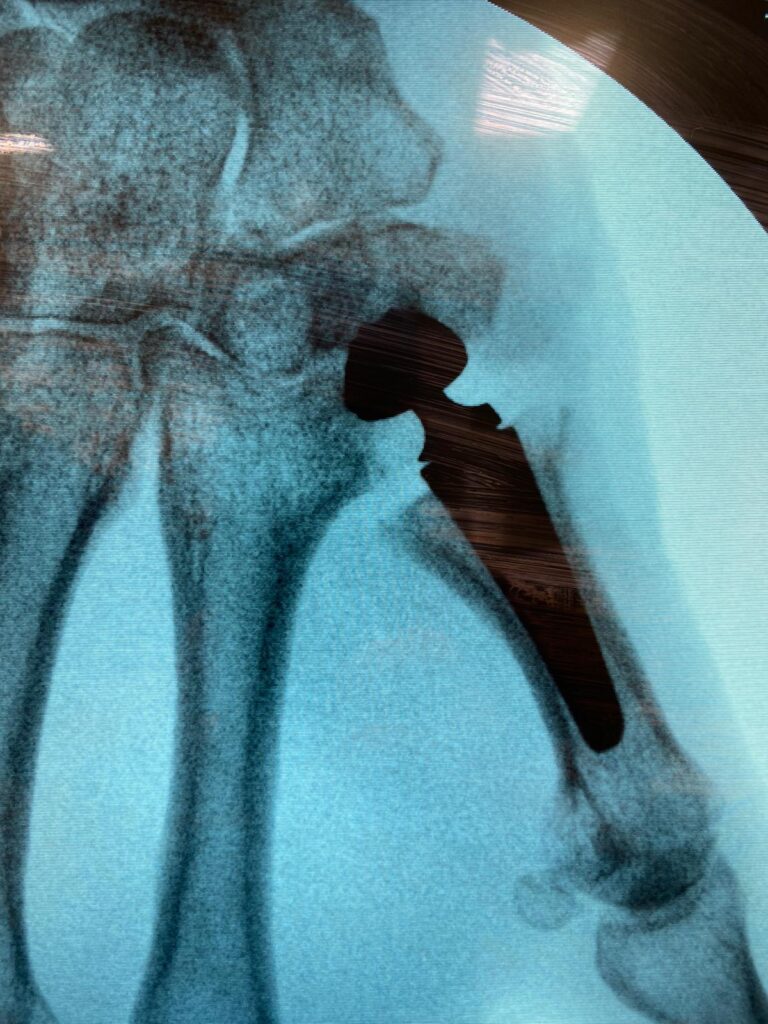
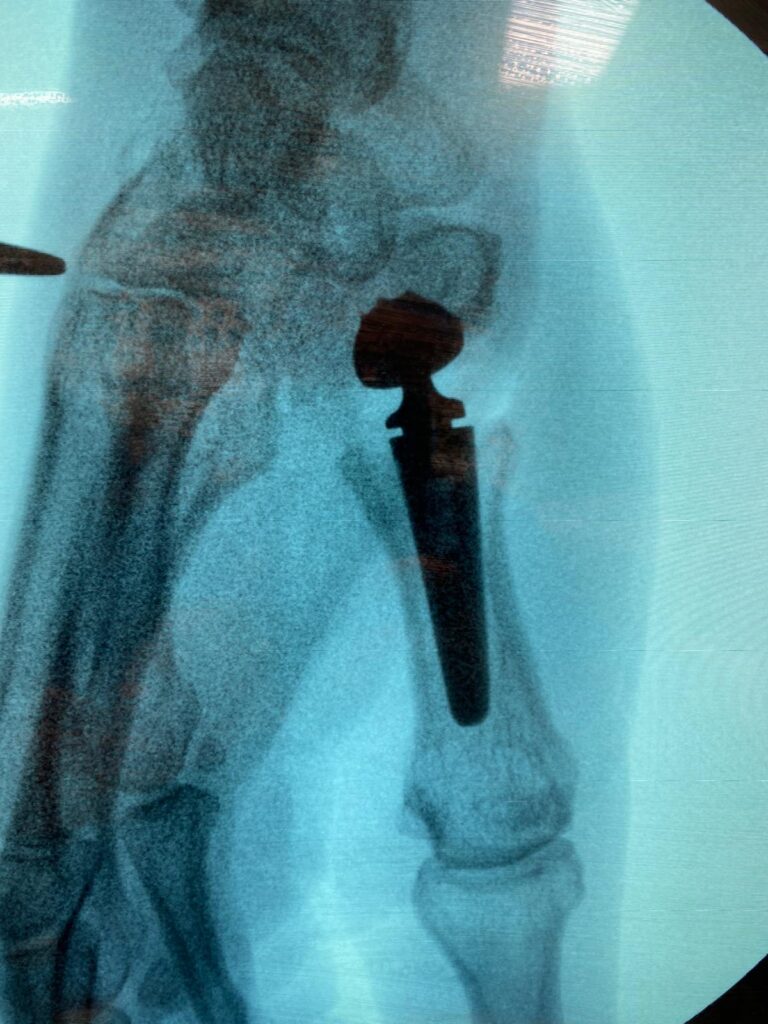
What happens after the surgery?
Taking simple painkillers such as paracetamol regularly for the first 2 days after the operation will help to relieve any post-operative pain. Stitches will be removed at 10-14 days after the operation either at your GP or at the hand clinic. Mr. Naqui and the hand therapist will provide you with specific exercises to perform after the surgery but early finger and thumb movements are advised. You will usually be required to wear a protective splint for a period of 4-6 weeks.
Watch Video
6 weeks after joint replacement surgery
When I can return to normal activity (work, driving, sports)?
If you perform lifting at work it is advised to stay off work for a period of 6-12 weeks dependent on the extent of lifting you do. If you work in an office a period of 1-2 weeks off work is sufficient provided you can work with a splint on your hand.
You are not advised to drive for 6-8 weeks after surgery.
Mr. Naqui will discuss your return to sport with you, depending on your requirements.
What are the complications of surgery?
Joint removal and ligament reconstruction is considered a reliable procedure. There may be persistent pain, weakness and stiffness post operatively. The risks of infection and nerve injury are small.