Mallet (Baseball) Finger
What is it?
Mallet finger is an injury to the tendon, which straightens the end joint (the distal inter-phalangeal joint or DIPJ) of a finger or thumb. It is sometimes referred to as baseball finger. Tendons are structures, which attach muscles to bone enabling us to move our joints.
Who gets it and what causes it?
This most commonly occurs following an injury to the tip of the finger, when the finger is stubbed and bent further than it should. This could happen following a simple fall on your hand, but very often is the result of the finger being struck during a ball game such as netball, cricket and football. In some inflammatory conditions such as rheumatoid arthritis it can occur with little or no injury.
Often patients present late to a hand specialist thinking that the injury is minor and will settle.
What are the signs and symptoms?
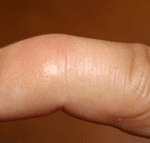
Patients may experience pain, swelling and bruising at the end joint of the finger. The fingertip classically droops downwards. On examining the finger, the joint can be corrected, only for it to droop down when let go of.
What tests will I need?
The first step is to undergo a consultation, involving a medical history and clinical examination. Mr Naqui may organise further tests such as an x-ray. An x-ray can reveal if there has been an associated fracture of the bone and what the position of the joint is like.
What is the treatment?
Treatment will depend on whether there is any fracture and how long ago the injury occurred.
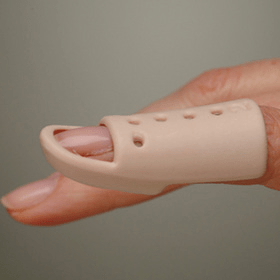
The first line treatment is usually to place the finger tip in a splint for a continuous period of 6 to 8 weeks which prevents movement of the end joint of the finger and allows the fractured bone or injured tendon to heal. To keep the finger in a splint for this length of time requires perseverance.
If there is a fracture and the joint is significantly out of position (subluxed), Mr Naqui may advocate surgery.
What does the surgical treatment involve?
Surgery is performed under a local anaesthetic, numbing the finger for a short period of time. A small wire is placed across to correct the position of the joint. Usually stitches are not required. You will be able to go home the same morning or afternoon
What happens after the surgery?
Taking simple painkillers such as paracetamol regularly for the first 2 days after the operation will help to relieve any post-operative pain.
Mr. Naqui and the hand therapist will then provide you with a specially adapted splint and specific exercises to perform to maintain normal movements in the rest of the hand.
The wire is usually left in position for 4 weeks, it is removed in clinic under local anaesthetic.
When I can return to normal activity?
Following splintage and tendon healing, you will be given formal exercises to regain full flexibility of the fingertip.
Activities which stress the finger should be avoided for up 3 months. Mr. Naqui will discuss with you regarding return to sports depending upon your particular sport – as a protective splint could be worn to help you get back to sport earlier. Driving can safely be resumed at around 4 weeks. Return to work is dependent on the nature of you work but usually expected within 2 weeks if it is non-manual work. You can discuss this with Mr Naqui at your consultation.
What are the complications of surgery?
The main potential complications that will be discussed with your prior to gaining consent for surgery include recurrence of deformity, pain, swelling, infection, stiffness, scarring and numbness.
Pain and swelling are common following surgery, these should settle after a few days with simple painkillers. Infection is rare. Stiffness at the joint should resolve if you follow the exercise programme as advised by Mr Naqui and the hand therapist following surgery.
In a proportion of patients tendon healing does not occur despite splintage and/ or wiring with a resultant re-droop of the finger. If this were to happen then there are further non-surgical and surgical options, which you can discuss with Mr Naqui.





